

Does Osteoporosis Cause Pain if There Are No Fractures?
No, osteoporosis does not directly cause pain if there are no fractures. Osteoporosis is fundamentally a metabolic skeletal disorder defined by reduced bone strength and an increased risk of fracture.
The condition develops from an imbalance between bone resorption and bone formation, leading to deterioration of the bone’s internal structure. Many people assume this weakening causes a constant dull ache or deep soreness in the bones.
In reality, bone tissue lacks the dense network of pain fibers found in surrounding structures, so this gradual breakdown does not directly trigger pain signals. The key clinical distinction is between pain caused by an actual fracture and discomfort that arises later from mechanical dysfunction in a weakened skeleton. Does osteoporosis cause pain if there are no fractures? Let's find out.

The Asymptomatic Nature of Bone Loss in Osteoporosis
Osteoporosis is often described as a silent disease, but this description reflects a specific anatomical and physiological reality rather than a general absence of pathology. The processes that weaken bone structure occur largely without activating the body’s pain detection systems, allowing significant deterioration to develop before any symptoms appear.
The Absence of Sensory Innervation Within Bone
Bone is a living tissue, but its internal structure lacks the components needed to transmit pain signals to the central nervous system. Nociceptors, which detect mechanical, thermal, or chemical damage, are located mainly in the periosteum, the dense outer membrane of the bone.
The trabecular interior and cortical bone contain very few of these nerve endings. As a result, gradual demineralization does not activate pain receptors.
Osteoclasts resorb bone and osteoblasts form new matrices without stimulating surface nerves. This separation explains why bone turnover remains a silent process even when resorption exceeds formation.
The Painless Nature of Microarchitectural Deterioration
The disease process involves a reduction in the connectivity of the trabecular plates and rods within the cancellous bone. This structural decay weakens the internal support system, but it does not produce a sensation of pain.
The collapse of these individual struts happens below the threshold of human perception.
- The loss of bone mineral density occurs gradually over years, allowing the body to adapt without sending distress signals.
- The microfractures that occur at the cellular level are too small to disturb the periosteum, which remains intact and unstimulated.
- There is no inflammatory component associated with simple bone thinning, unlike arthritis which involves swollen and irritated joint linings that press against sensitive tissues.
The Periosteum as the Threshold for Sensation
The periosteum serves as the critical boundary between silent pathology and conscious pain. This membrane contains a rich network of sensory nerves that respond to stretching, tearing, or impact.
In the absence of a fracture that disrupts this outer layer, the weakened bone underneath can continue to deteriorate without ever engaging these sensitive nerve fibers. For a patient to feel direct bone pain, the structural failure must extend to the surface where the nerves reside.
A non-displaced vertebral fracture or a crack in the cortical bone will stretch the periosteum and generate a sharp, localized signal. Until that mechanical event occurs, the disease remains hidden from the patient's sensory awareness.
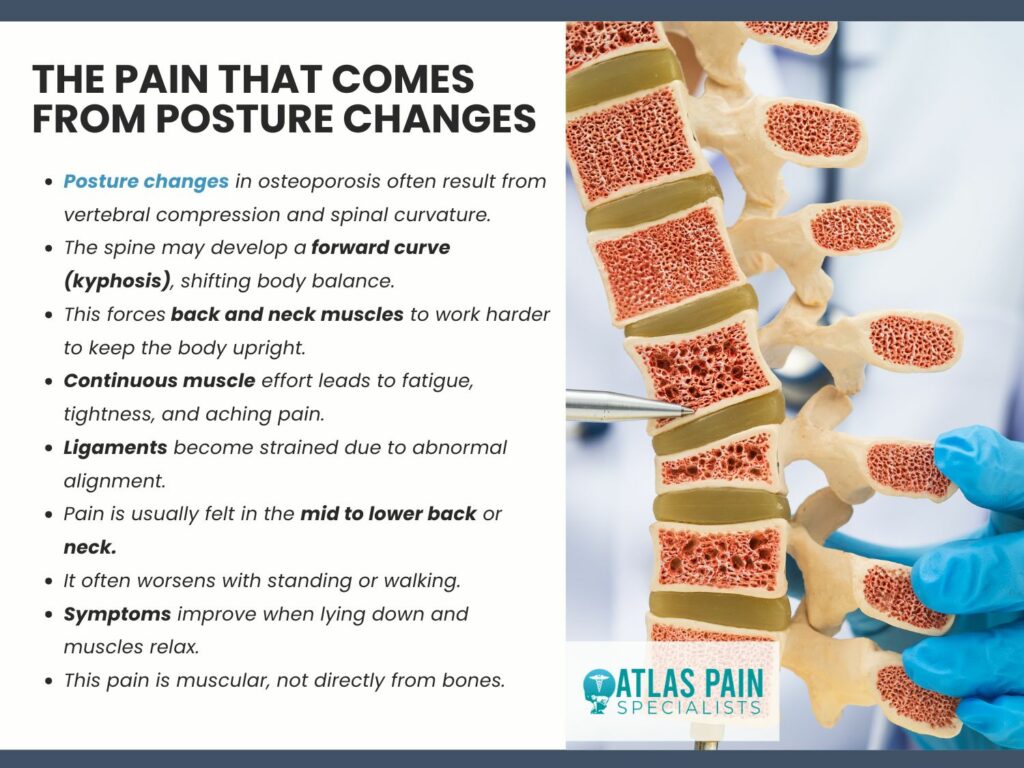
The Pain That Comes From Posture Changes
As osteoporosis progresses, structural changes within the spine can lead to significant alterations in posture. These changes do not directly cause bone pain but instead create secondary mechanical strain on muscles, ligaments, and joints, resulting in persistent discomfort and functional limitations.
- The Biomechanical Shift of Vertebral Collapse
The thoracic spine supports the weight of the upper body and maintains the upright position against gravity. When multiple vertebral bodies lose height due to compression fractures, even those that go undiagnosed, the natural alignment of the spinal column shifts forward.
This creates an increased thoracic kyphosis, a curvature that forces the head and neck to extend backward to maintain a horizontal gaze. This realignment places the center of mass anterior to the pelvis.
The body compensates by recruiting posterior chain muscles to prevent a forward fall. The paraspinal muscles, erector spinae, and deep stabilizers must work continuously to counteract this force, leading to fatigue and localized tenderness.
- Compensatory Muscle Strain and Ligamentous Stress
The soft tissues surrounding the spine were not designed to bear the load created by a severely curved posture. Ligaments along the anterior portion of the spine become slack while those in the posterior are placed under constant tension
- The cervical extensors contract forcefully to keep the head level, which often results in tension headaches and upper neck pain.
- The lumbar erector spinae work excessively to stabilize the lower back, as the thoracic curve above disrupts the efficient transfer of load through the vertebral column.
The costovertebral joints, where the ribs attach to the spine, can become irritated from the altered thoracic shape, producing a dull ache near the shoulder blades that mimics lung or cardiac referral patterns.
- Pain Originating From Overworked Muscles
The sensation experienced by many individuals with advanced osteoporosis is not bone pain but myofascial pain from constantly contracted muscles. These muscles accumulate metabolic waste and develop trigger points due to the ongoing effort required to maintain posture.
Patients often describe a burning sensation along the spine or a deep ache in the lower back that worsens throughout the day. This pain follows the pattern of overworked muscles rather than a specific dermatome.
The discomfort improves with lying down, which reduces gravitational load and allows the muscles to relax. It returns upon standing as the muscles resume compensating for the altered spinal alignment.
The Difference Between a Fracture and a Micro-Fracture
Bone damage presents in different forms, and understanding the difference between a full fracture and a micro-fracture is critical for interpreting symptoms. Both involve structural compromise, but they differ significantly in severity, visibility on imaging, and the type of pain they produce.
This distinction becomes especially important in conditions like osteoporosis, where bone weakening occurs gradually.
- The Clinical Fracture Event
A clinical fracture represents a complete or partial break in the bone that is visible on standard radiographs. It involves disruption of the cortical bone and often includes displacement of bone fragments.
The mechanical failure is severe enough to stretch or tear the periosteum, which contains a dense network of pain fibers. This produces a sharp and localized pain signal.
Pain from a fracture is acute and closely linked to movement. Weight bearing becomes difficult or impossible, and surrounding muscles tighten to limit motion while the pain gradually improves as healing occurs.
- The Nature of Micro-Fractures in Weakened Trabeculae
Micro-fractures, sometimes called microfissures or stress reactions, occur within individual trabeculae in the cancellous bone. These tiny cracks do not extend through the full thickness of the bone or disrupt the outer cortical surface.
In healthy bone, these micro-fractures heal through normal remodeling without producing symptoms. In osteoporotic bone, the rate of accumulation exceeds the capacity for repair.
The trabecular network becomes weakened and inefficient at transmitting forces. These small failures create localized bone edema and mild inflammation within the marrow, which can generate a low-level pain signal.
- Differentiating Pain Quality and Presentation
The sensory experience of a micro-fracture differs substantially from that of a complete fracture. Patients do not report a sudden, sharp pain associated with a specific incident.
Instead, they describe a diffuse, dull ache located deep within a region, such as the hip or the low back, that appears during sustained weight bearing and fades with rest.
- The pain tends to be activity-dependent rather than constant, appearing after walking for a certain distance or standing for prolonged periods.
- There is no single point of tenderness that the patient can identify with a finger, as the discomfort arises from a region of accumulated micro-damage rather than a single disrupted site.
Percussion over the bone may reproduce a mild ache, but it does not elicit the sharp wincing response seen with a true fracture.
How Spinal Changes Cause Abdominal Discomfort
Advanced osteoporosis affects more than bone strength alone; it alters the structural relationships within the torso. As vertebral compression fractures change the shape of the spine, they reduce space in the chest and abdomen, placing pressure on internal organs and causing digestive and breathing symptoms.
The Anatomical Consequences of Thoracic Kyphosis
The thoracic spine forms the posterior wall of the chest cavity and provides the attachment points for the ribs. When multiple vertebral compression fractures occur in the mid to lower thoracic region, the spinal column shortens and curves forward.
This collapse reduces the vertical dimension of the thorax, forcing the rib cage downward toward the iliac crests of the pelvis. The space available for the abdominal viscera becomes constrained.
The stomach, the transverse colon, and the small intestine normally occupy a volume that depends on adequate separation between the diaphragm and the pelvic floor. As the rib cage descends, it compresses the abdominal contents against the pelvic basin, leaving less room for distention after meals and less space for normal peristaltic movement.
Gastrointestinal Symptoms From Mechanical Compression
Patients with significant height loss from osteoporosis frequently report a cluster of digestive complaints that have no primary gastrointestinal pathology. These symptoms arise purely from the altered geometry of the trunk and the resulting pressure on hollow organs.
- Early satiety occurs because the stomach cannot expand fully when compressed between the diaphragm and the anterior abdominal wall, leading to a sensation of fullness after only small amounts of food.
- Gastric reflux increases as the intra-abdominal pressure rises, pushing gastric contents against a lower esophageal sphincter that now sits at a different angle relative to the stomach.
- Constipation develops from mechanical slowing of colonic transit, as the descending colon must navigate a shortened and crowded abdominal cavity.
- Bloating and abdominal distention appear after meals as swallowed air and digestive gases have limited space to disperse.
The Sensation of Pain Referred to the Abdomen
The discomfort associated with these mechanical changes does not originate from the spine itself but from the viscera under pressure. Patients often describe a vague, pressure-like ache in the upper abdomen or around the flanks that they cannot localize precisely.
This sensation differs from the sharp, movement-related pain of a vertebral fracture. The phrenic nerve and the lower intercostal nerves innervate both the diaphragm and the peritoneum.
When the descending rib cage irritates these structures, the brain can misinterpret the signal as originating from the upper abdominal organs. This referred pattern leads some patients to undergo evaluations for gallbladder disease or peptic ulcers when the true cause is the postural collapse of their osteoporotic spine.
Back Hurts When I Sneeze: Is It Normal or a Sign of Something More?
Osteoporosis remains a silent condition until the skeleton reaches a point where it can no longer handle normal mechanical stress without damage. The symptoms people feel are not caused by bone loss itself but by the effects that follow, including structural changes and fractures.
A sudden sharp pain in the back during a sneeze clearly demonstrates this. The force created by the movement, along with muscle contraction, is normally well tolerated by a healthy spine.
When that same force causes immediate localized pain in someone with osteoporosis, it suggests that the vertebra has likely failed. What seems like a simple reflex becomes an important sign that requires medical evaluation.
About Dr. Sean Ormond



