
Sacroiliac Joint Injection Recovery Time: What Patients Should Know
Recovery after a sacroiliac joint injection is usually quick, with most patients returning to normal activities within a few days, though full pain relief may take one to three weeks. The exact timeline depends on your body, the severity of your condition, and how well you follow post-procedure care instructions.
Many patients are surprised by how manageable the recovery process is, especially when they know what to expect ahead of time. In most cases, sacroiliac joint injection recovery time is short, but the full benefits develop gradually as inflammation decreases and healing progresses.
Understanding this timeline helps you plan daily activities, avoid unnecessary strain, and feel more confident about the procedure. This guide breaks down each stage of recovery, key influencing factors, and practical ways to support better outcomes.
What Is a Sacroiliac Joint Injection and Why Is It Done?
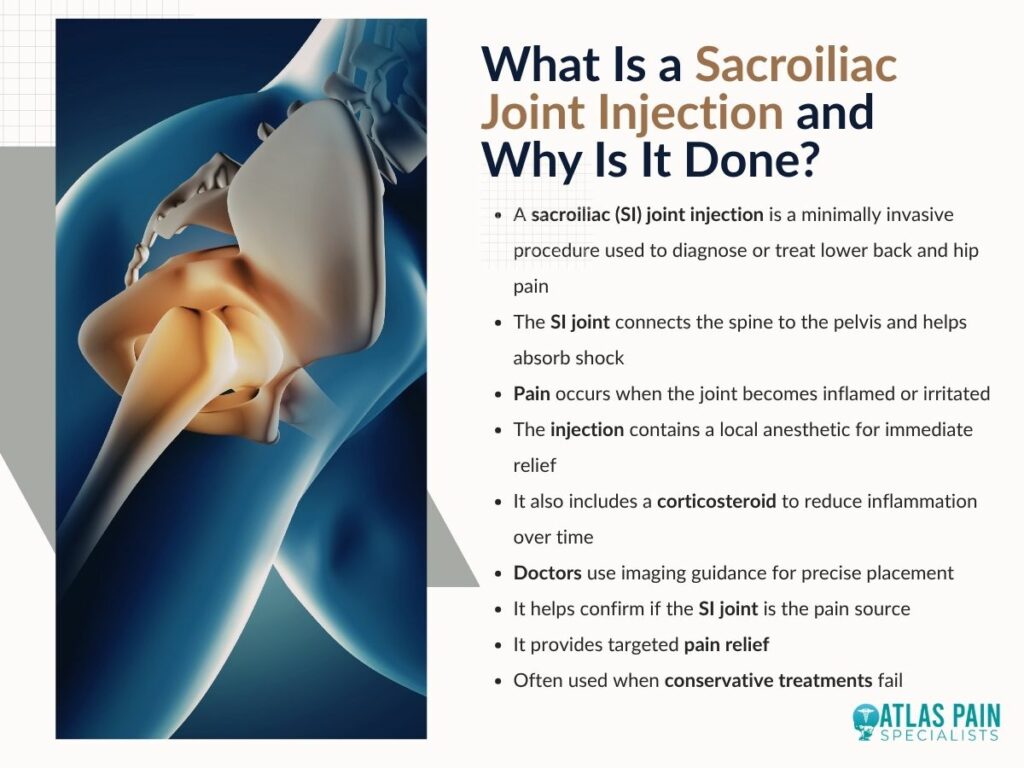
The sacroiliac joint connects the lower spine to the pelvis and plays a key role in absorbing shock and stabilizing movement. When this joint becomes inflamed or irritated, it can lead to persistent lower back and hip pain that may radiate into the legs.
A sacroiliac joint injection is a minimally invasive procedure used to diagnose or treat this pain. The injection typically contains a combination of a local anesthetic and a corticosteroid.
The anesthetic provides immediate but temporary relief, while the steroid works over time to reduce inflammation. Doctors often use imaging guidance to ensure the medication is delivered precisely into the joint space.
A sacroiliac joint injection serves both as a diagnostic tool and a targeted treatment for chronic lower back pain.
Conditions That May Require an SI Joint Injection
Several underlying issues can lead to sacroiliac joint pain. These include sacroiliitis, which is inflammation of the joint, and degenerative arthritis that develops over time. Injuries, such as falls or car accidents, can also disrupt the joint’s stability.
Pregnancy is another contributing factor due to hormonal changes that loosen ligaments around the pelvis. In some cases, pain originates from abnormal movement patterns that strain the joint repeatedly. Identifying the cause helps determine whether an injection is the right solution.
What Happens During the Procedure
The procedure is usually performed in an outpatient setting and takes less than 30 minutes. Patients lie face down while a physician uses fluoroscopy or CT imaging to guide a needle into the sacroiliac joint. After confirming proper placement, the medication is injected.
Most patients experience minimal discomfort during the process, especially when they understand what to expect from a pain management doctor before and during the procedure.
You may feel slight pressure or a brief stinging sensation, but sedation is rarely required. Once completed, patients are monitored briefly before being allowed to go home the same day.
Sacroiliac Joint Injection Recovery Time Explained
Recovery after the injection happens in stages, beginning immediately after the procedure and continuing over the following weeks. While many patients feel some relief right away due to the anesthetic, this effect wears off within hours.
The steroid component takes longer to reduce inflammation and provide lasting results. It is normal to experience mild soreness at the injection site, which typically resolves within a day or two.
Some patients may even notice a temporary increase in pain before improvement begins. This is part of the body’s response to the injection and usually subsides quickly.
Recovery after an SI joint injection is typically fast, but meaningful pain relief often builds gradually over several days.
Immediate Post-Procedure Recovery (First 24 Hours)
During the first day, you may feel numbness or weakness in the lower back or legs due to the anesthetic. This is temporary and should fade within a few hours.
Mild tenderness at the injection site is common and can be managed with rest. Patients are usually advised to avoid strenuous activity during this period and follow guidelines on what to avoid after a pain injection to prevent unnecessary irritation.
Light walking is acceptable, but heavy lifting or intense exercise should be postponed. Along with rest and ice application, you can also improve comfort during recovery by adopting proper sleeping positions for sacroiliac joint pain, which help reduce strain on the joint.
Short-Term Recovery (2 to 7 Days)
As the anesthetic wears off, some patients experience a brief return of pain. This can feel discouraging but is expected. The steroid medication begins working during this phase, gradually reducing inflammation in the joint.
Most people can resume normal daily activities within a couple of days. However, it is wise to ease back into physical routines rather than jumping in at full intensity. Paying attention to how your body responds is key to avoiding setbacks.
Long-Term Results (1 to 3 Weeks)
By the end of the first week, many patients begin to notice significant improvement in their symptoms. Pain levels decrease, mobility improves, and daily tasks become easier. Full benefits are often felt within two to three weeks.
If relief is minimal or short-lived, your doctor may reassess the diagnosis or recommend additional treatments. In some cases, repeat injections or physical therapy may be part of a broader care plan.
Common Side Effects During Sacroiliac Joint Injection Recovery
Understanding what your body might experience after the procedure helps reduce anxiety and ensures you respond appropriately to normal symptoms. While sacroiliac joint injections are generally safe, mild side effects are fairly common and typically short-lived.
These reactions are part of the body’s natural response to both the injection itself and the medication used. Most side effects occur within the first few days and gradually fade without intervention.
However, knowing the difference between expected discomfort and something that needs medical attention is important. Patients who are well-informed tend to recover more confidently and avoid unnecessary worry.
Most side effects after an SI joint injection are mild, temporary, and resolve within a few days without treatment.
Common Side Effects You May Experience
Here are the most frequently reported post-injection symptoms:
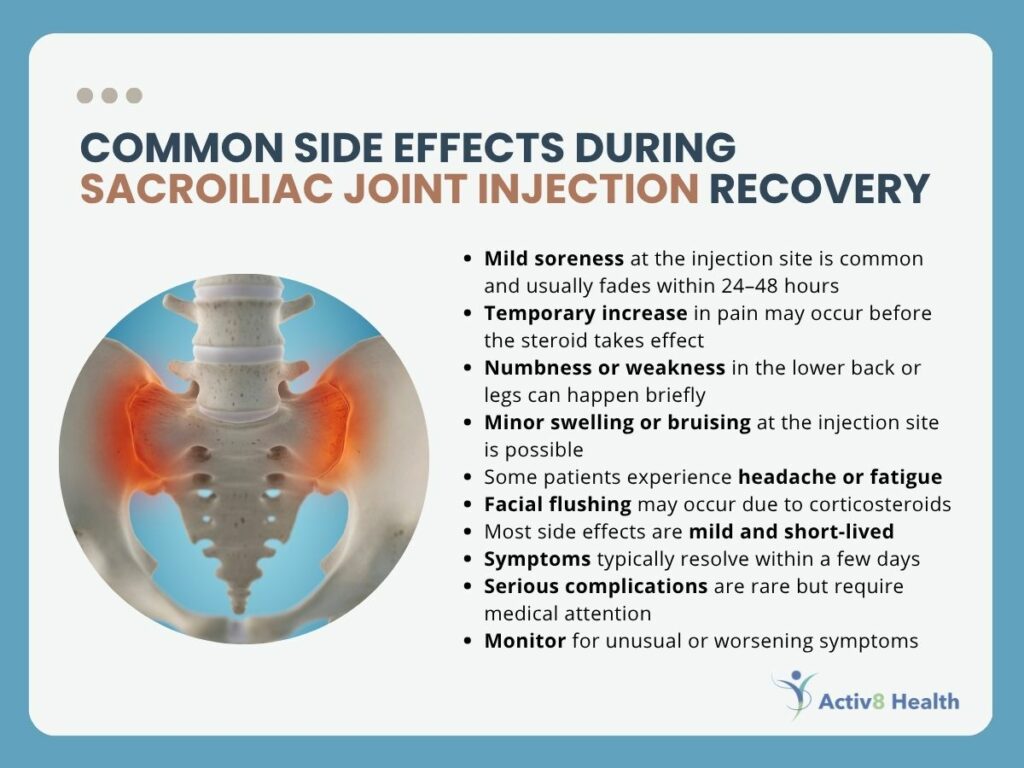
- Soreness at the Injection Site
Mild pain or tenderness where the needle was inserted is the most common complaint. This usually improves within 24 to 48 hours and can be managed with ice packs.
- Temporary Increase in Pain
Some patients experience a short-term flare-up before the steroid begins working. This can last a few days but is not a cause for concern.
- Numbness or Weakness
The anesthetic used during the injection may cause temporary numbness in the lower back or legs. This effect typically wears off within a few hours.
- Mild Swelling or Bruising
Slight swelling or bruising at the injection site may occur but generally resolves quickly.
- Headache or Fatigue
A small number of patients report feeling tired or developing a mild headache after the procedure.
- Facial Flushing from Steroids
Corticosteroids can sometimes cause temporary warmth or redness in the face, which fades within a day or two.
When Side Effects May Require Attention
Although rare, certain symptoms should not be ignored. Severe pain that worsens over time, signs of infection such as fever or redness, or prolonged numbness should be evaluated by a healthcare provider.
A 2020 review published in Pain Physician Journal found that serious complications from joint injections are uncommon, occurring in less than 1 percent of cases. This reinforces that most recovery experiences are straightforward and manageable.
Being aware of these potential side effects allows you to stay calm and focused during recovery. It also helps you distinguish between normal healing and situations that require medical input.
Factors That Affect Recovery Time
Not all patients recover at the same pace, especially since underlying conditions and the causes of lower back and hip pain can vary from person to person.
Several factors influence how quickly you feel better and how long the relief lasts. Understanding these variables can help set realistic expectations.
Your overall health plays a major role in recovery. Individuals with chronic conditions or inflammation elsewhere in the body may take longer to respond. Age, fitness level, and previous injuries also contribute to healing speed.
Recovery time varies because each patient’s condition, lifestyle, and response to treatment are unique.
- Personal Health and Medical History
Patients with conditions such as arthritis or obesity may experience slower improvement due to ongoing joint stress. Previous lower back injuries can also complicate recovery by affecting surrounding structures.
A 2022 report from the American Academy of Orthopaedic Surgeons noted that patients with multiple musculoskeletal conditions often require longer recovery periods and more comprehensive treatment plans.
- Activity Level After the Procedure
How you move after the injection matters. Too much rest can lead to stiffness, while overexertion can aggravate the joint. Finding a balance between gentle movement and adequate rest supports healing.
Gradual reintroduction of activity is usually recommended. Walking, stretching, and low-impact exercises can help maintain mobility without placing excessive strain on the joint.
- Response to Steroid Medication
Not everyone responds to corticosteroids in the same way. Some patients feel relief within a few days, while others may need more time. The duration of pain relief also varies, ranging from weeks to several months.
Your doctor may use your response to the injection to guide future treatment decisions. If the injection provides significant relief, it confirms the sacroiliac joint as the source of pain.
Tips for a Smooth and Faster Recovery
Supporting your body after the procedure can make a noticeable difference in how quickly you recover. Simple habits and precautions help reduce discomfort and improve outcomes.
Proper post-procedure care is not complicated, but consistency matters. Following your doctor’s instructions and listening to your body are the most effective ways to promote healing.
Small, consistent actions after the injection can significantly improve recovery speed and overall results.
Do’s and Don’ts After the Injection
Here are a few practical guidelines to follow:
- Rest during the first 24 hours after the procedure
- Apply ice to the injection site if soreness develops
- Avoid heavy lifting or intense exercise for several days
- Stay hydrated and maintain a balanced diet
- Gradually return to normal activities as pain allows
These steps help minimize irritation and support the healing process without overloading the joint.
When to Resume Normal Activities
Most patients can return to light activities within one to two days. Desk work and routine tasks are usually manageable shortly after the procedure. More physically demanding activities should be reintroduced slowly over the following week.
Exercise programs, especially those involving the lower back, should be resumed under guidance. Physical therapy may be recommended to strengthen supporting muscles and prevent recurrence of pain.
Warning Signs to Watch For
While complications are rare, it is important to be aware of potential warning signs. Severe pain, swelling, or redness at the injection site should not be ignored. Fever or unusual symptoms may indicate infection.
Persistent numbness or weakness beyond the first day also warrants medical attention. Prompt communication with your healthcare provider ensures any issues are addressed early.
How to Maximize Pain Relief After an SI Joint Injection
Getting the injection is only part of the process. What you do afterward plays a significant role in how effective the treatment will be. Patients who actively support their recovery often experience longer-lasting and more meaningful pain relief.
The goal is not just to reduce pain temporarily but to improve joint function and prevent future flare-ups. This involves a combination of movement, posture awareness, and healthy daily habits. Small adjustments can make a noticeable difference over time.
Maximizing the benefits of an SI joint injection depends largely on consistent post-procedure habits and lifestyle choices, often supported by personalized pain management plans tailored to your condition.
Strategies to Improve and Extend Pain Relief
- Follow a Guided Physical Therapy Plan
Strengthening the muscles around the pelvis and lower back helps stabilize the sacroiliac joint. A structured program can prevent recurring pain.
- Maintain Good Posture Throughout the Day
Sitting or standing incorrectly places unnecessary stress on the SI joint. Keeping your spine aligned reduces strain and supports healing.
- Use Heat or Ice Appropriately
Ice works best in the early days to reduce inflammation, while heat can help relax muscles later in recovery.
- Avoid High-Impact Activities Initially
Running, jumping, or heavy lifting can irritate the joint. Gradually reintroducing these activities prevents setbacks.
- Incorporate Low-Impact Exercise
Walking, swimming, and gentle stretching improve circulation and keep joints mobile without excessive stress.
- Manage Body Weight if Necessary
Extra weight increases pressure on the lower back and pelvis. Maintaining a healthy weight supports long-term joint health.
- Stay Consistent With Follow-Up Care
Attending follow-up appointments ensures your progress is monitored and adjustments are made if needed.
Why Lifestyle Changes Matter
Pain relief from the injection can last weeks or even months, but without supportive habits, symptoms may return. A 2021 report from the Centers for Disease Control and Prevention highlighted that lifestyle factors play a major role in managing chronic musculoskeletal pain.
This means recovery is not just about healing from the procedure but also about preventing future irritation. Patients who combine medical treatment with lifestyle improvements tend to see the best long-term outcomes.
By taking an active role in your recovery, you turn a short-term procedure into a more lasting solution for managing sacroiliac joint pain.
Comparing SI Joint Injection Recovery With Other Back Treatments
Understanding how this procedure compares to other treatments helps put recovery expectations into perspective. Sacroiliac joint injections are often chosen because they offer a balance of effectiveness and minimal downtime.
Unlike surgical options, injections do not require long recovery periods or hospitalization. Compared to physical therapy alone, they can provide faster relief, especially when inflammation is severe.
SI joint injections offer a shorter recovery time compared to many other back pain treatments, making them a practical first step.
| Treatment Type | Recovery Time | Invasiveness | Pain Relief Timeline |
| SI Joint Injection | Few days to 2 weeks | Minimally invasive | Days to weeks |
| Physical Therapy | Ongoing | Non-invasive | Gradual improvement |
| Spinal Surgery | Weeks to months | Highly invasive | Long-term recovery |
A 2021 study published by the National Institutes of Health found that minimally invasive treatments like joint injections often lead to quicker functional recovery compared to surgical interventions. This makes them a preferred option for many patients seeking relief without extended downtime.
Sacroiliac joint injection recovery time and What Comes Next
Understanding sacroiliac joint injection recovery time helps you approach treatment with realistic expectations and a clear plan. Most patients experience gradual improvement within the first week, with continued progress over the following weeks.
While the procedure itself is straightforward, recovery depends on how well you support your body afterward. For those who experience lasting relief, the next step often involves strengthening and maintaining joint stability through targeted exercises or physical therapy.
If pain returns, additional injections or alternative treatments may be considered. Exploring long-term strategies for managing lower back pain naturally leads into a broader conversation about prevention, posture, and lifestyle adjustments, as well as understanding long-term pain management strategies that support lasting relief..
About Dr. Sean Ormond



