Understanding Platelet-Rich Plasma (PRP) Therapy and Its Advantages
This treatment has gained recognition among patients looking for longer-term solutions to pain and mobility limitations caused by musculoskeletal wear, joint degeneration, and soft-tissue injury. Rather than simply masking symptoms, PRP focuses on improving the condition of the affected tissue itself.
At Atlas Pain Specialists, PRP is offered as part of a comprehensive, minimally invasive pain-care strategy. With offices in Glendale and Scottsdale, the clinic serves patients across the Phoenix Metro area, providing same-day appointments, accepting most major insurance plans and Medicare, and offering flexible self-pay options to make advanced pain care accessible.
What Is Platelet-Rich Plasma Therapy?
Once activated, these platelets release signaling proteins that support tissue repair, collagen formation, and inflammatory control. Because PRP is derived entirely from the patient’s own blood, it is considered a natural and low-risk treatment option that has been incorporated into many interventional and regenerative pain programs.
SCS is particularly beneficial for patients with persistent nerve pain, such as those caused by failed back surgery syndrome, complex regional pain syndrome (CRPS), and neuropathic pain conditions. It offers a customizable approach, allowing patients and physicians to adjust stimulation levels based on individual needs. Many patients experience a significant reduction in pain and an improved quality of life, regaining mobility and independence that was previously limited by chronic pain.
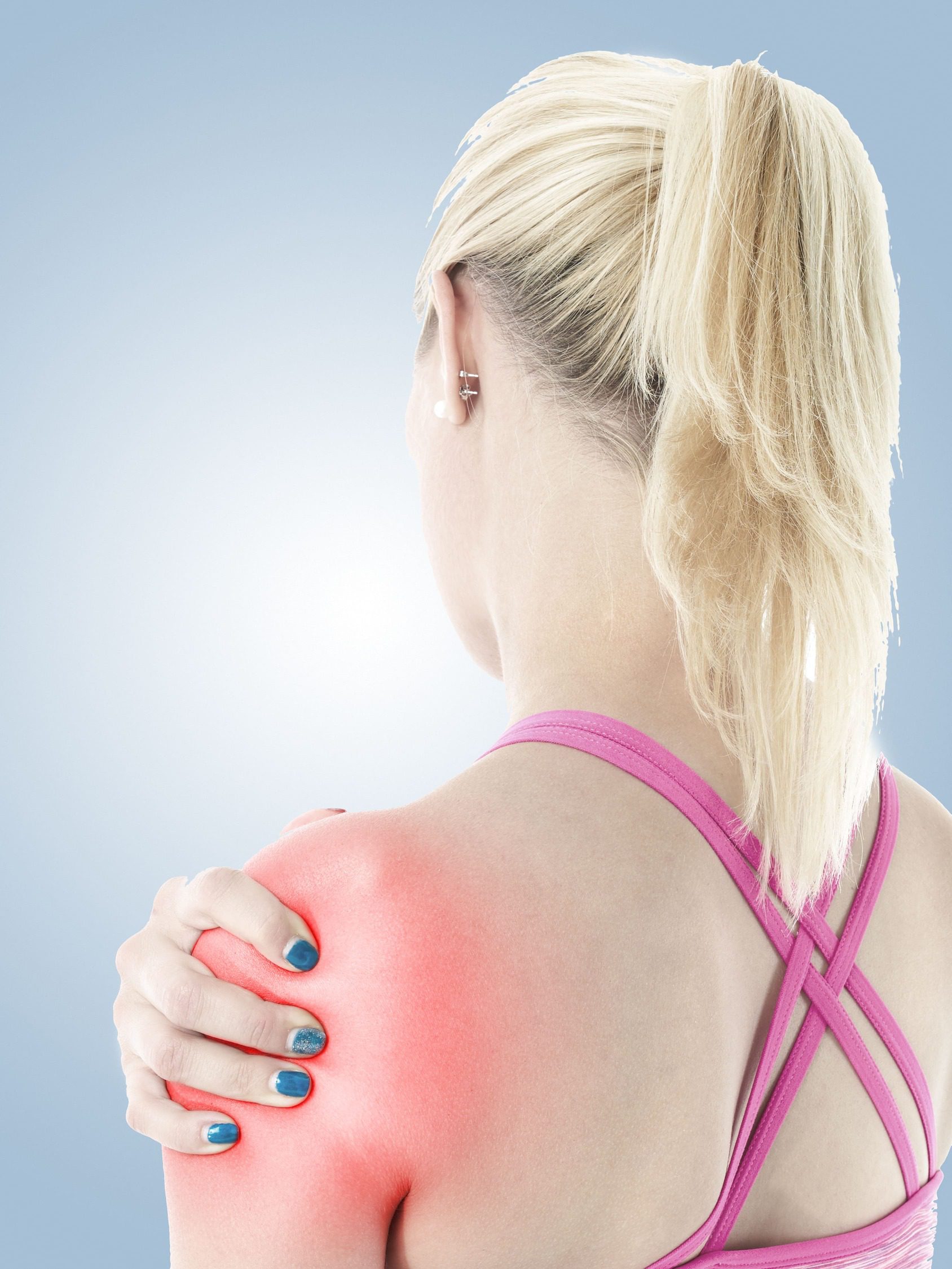
Conditions That May Be Treated With PRP
Conditions Commonly Addressed With PRP
What to Expect
Effectiveness
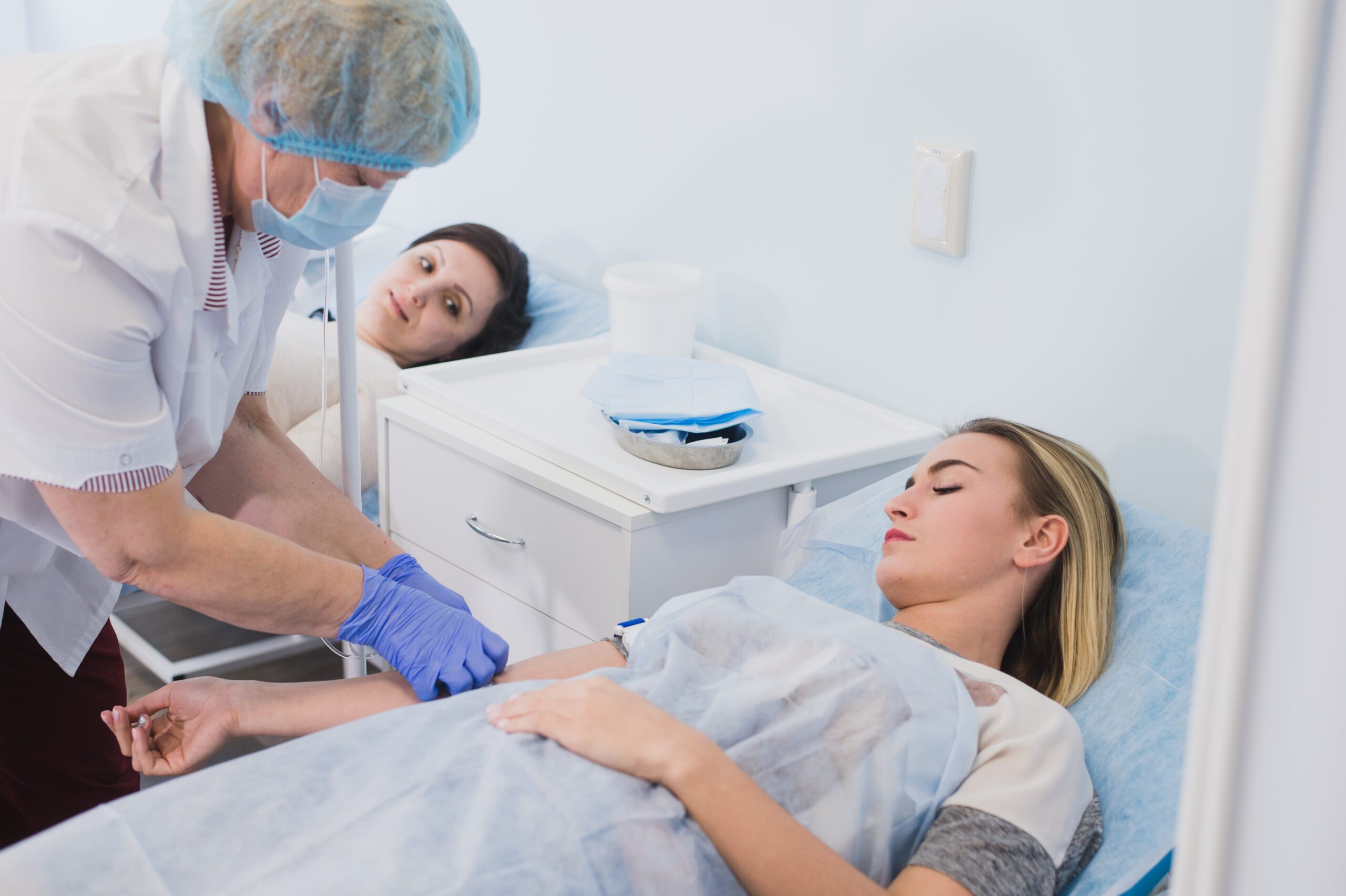
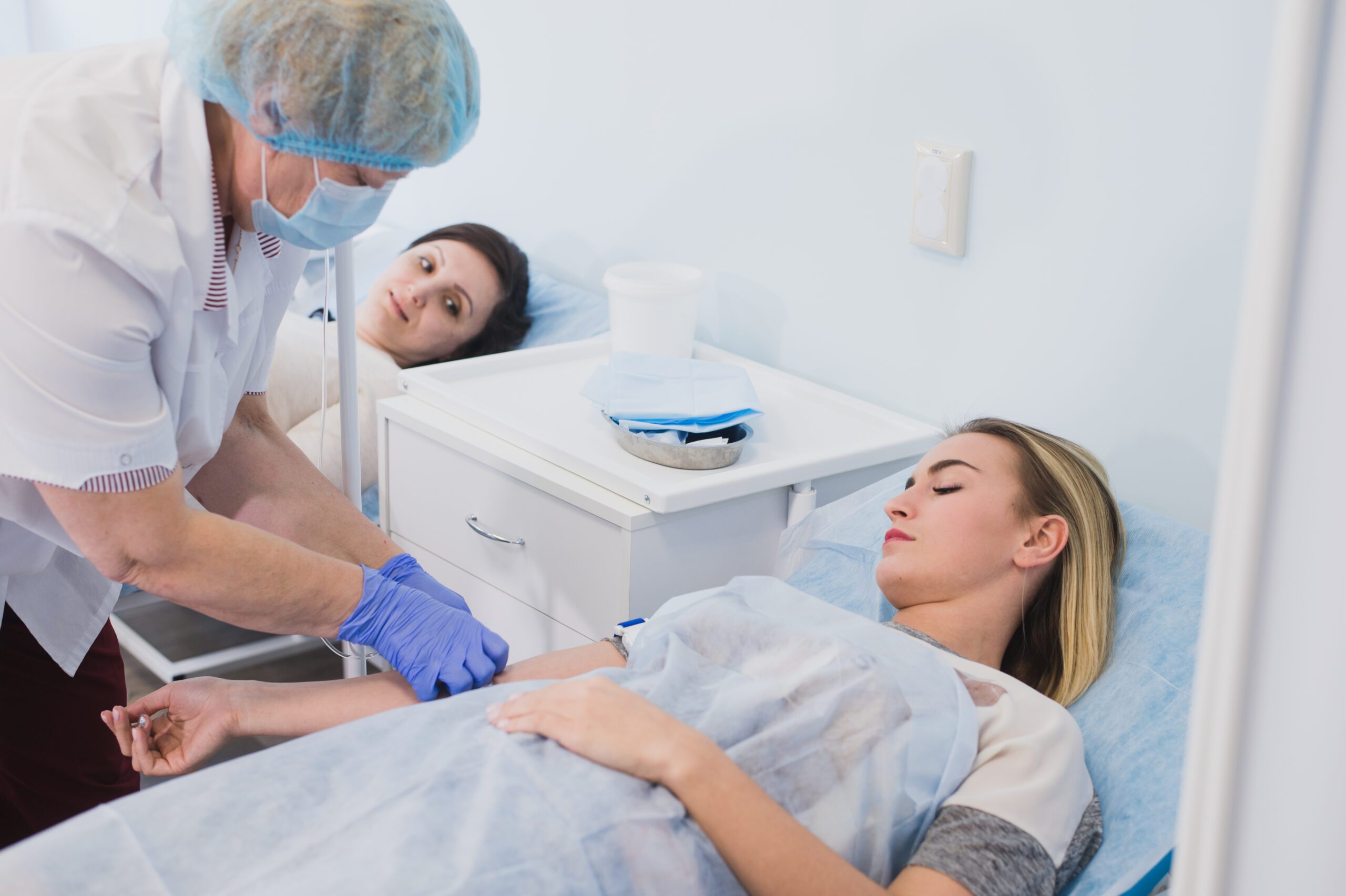
What to Expect During the PRP Procedure
The PRP procedure is straightforward and performed on an outpatient basis. After drawing blood from the patient’s arm, the sample is processed to concentrate the platelets. The prepared PRP is then carefully injected into the targeted area.
Since the treatment uses the patient’s own biological material, the likelihood of adverse reactions is low. Most appointments are completed in under an hour, allowing patients to return home the same day.
Results and Effectiveness of PRP Therapy
PRP therapy works by encouraging the body’s natural repair mechanisms, which means results develop gradually rather than immediately. Over time, patients may experience reduced pain, improved stability, and increased range of motion.
This treatment has been especially useful for chronic joint pain, spinal conditions, soft-tissue injuries, and early-stage osteoarthritis. PRP offers a regenerative option that fits between traditional conservative care and surgical intervention, helping many patients restore daily function with greater comfort.

Potential Risks of Spinal Cord Stimulation
As with any medical procedure, SCS carries some risks, though complications are rare. Some potential risks include:
- Infection – Though uncommon, an infection at the implant site may require removal of the device.
- Lead Migration – The electrodes may shift over time, leading to reduced effectiveness and requiring adjustment or repositioning.
- Device Malfunction – Though rare, mechanical failures in the device may require replacement.
- Tissue Irritation – Some patients experience mild discomfort or sensitivity around the implant site.
- Inconsistent Pain Relief – While many patients experience significant relief, results can vary, and some may not achieve the expected level of improvement.
The Spinal Cord Stimulation Process
The SCS procedure involves two main phases: the trial phase and the permanent implant.
- Trial Phase – A temporary SCS device is implanted using a minimally invasive technique. The patient wears an external stimulator for about a week to determine if the therapy provides significant pain relief.
- Evaluation – If the trial is successful (typically at least 50% pain reduction), the patient moves on to permanent implantation.
- Permanent Implantation – A small pulse generator is implanted under the skin, typically near the lower back or abdomen, and connected to leads placed near the spinal cord.
- Device Programming – The device is programmed to deliver customized electrical impulses, which the patient can adjust based on their pain levels.
- Recovery & Follow-Up – Patients typically return to light activity within a few days and receive regular follow-ups to optimize the device’s settings.
Types of Spinal Cord Stimulators
There are different types of SCS devices, each designed to meet the unique needs of the patient:
- Traditional Spinal Cord Stimulators – Deliver mild electrical impulses that replace pain signals with a tingling sensation (paresthesia).
- Burst Stimulation Devices – Use burst pulses to mimic natural nerve firing patterns, often reducing pain without causing a tingling sensation.
- High-Frequency Stimulators – Offer pain relief without paresthesia, making them ideal for patients who find tingling sensations uncomfortable.
- Rechargeable vs. Non-Rechargeable Devices – Rechargeable models provide longer battery life and more flexibility, while non-rechargeable versions require replacement every 5-10 years.
Each patient’s condition, preferences, and lifestyle determine which type of SCS system will provide the best long-term pain relief.
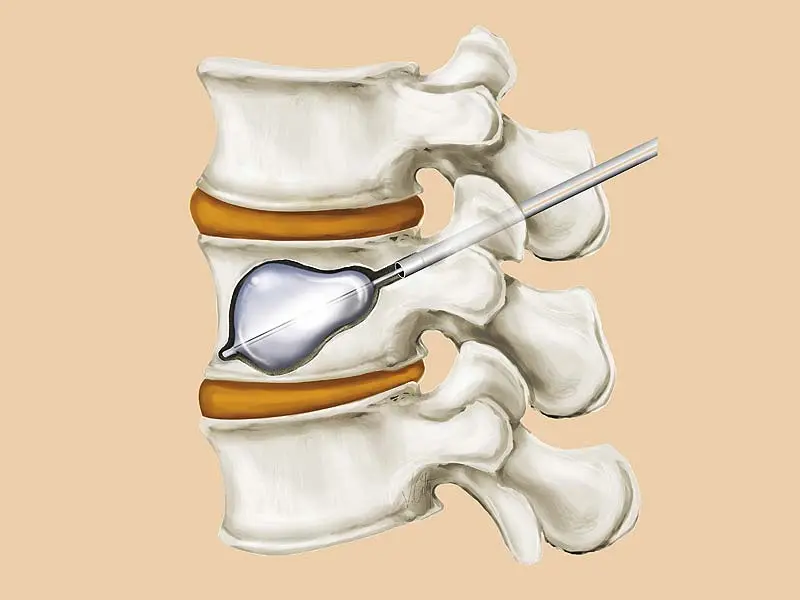
Types of Vertebral Compression Fractures Treated with Kyphoplasty
Kyphoplasty is most effective for acute or subacute compression fractures, meaning fractures that are relatively recent and still causing pain. Some of the common types include:
- Wedge fractures: The front of the vertebra collapses, creating a wedge-like shape and leading to kyphosis (hunchback posture).
- Biconcave fractures: The middle of the vertebra collapses, causing the bone to become concave in appearance.
- Crush fractures: The entire vertebra collapses uniformly, which can lead to severe instability.
The type and severity of the fracture determine whether kyphoplasty or another treatment approach is best.
Downloadable PDFs
Biological Principles and Clinical Applications
Choosing the Right Clinic for PRP Treatment
At Atlas Pain Specialists, patients receive physician-led care at every visit, ensuring precise diagnosis and customized treatment planning. The clinic’s focus on minimally invasive solutions, fast access to care, and patient-centered service makes it a trusted provider for PRP therapy in the Phoenix area.
Ask us anything, or
schedule a same day
appointment.
Accepted Insurances
References
Gupta S., Paliczak A., Delgado D. “Evidence-based indications of platelet-rich plasma therapy.” Expert Review of Hematology. 2020. DOI:10.1080/17474086.2021.1860002. Link: https://www.tandfonline.com/doi/full/10.1080/17474086.2021.1860002
Fang J., Wang X., Jiang W., et al. Platelet-Rich Plasma Therapy in the Treatment of Diseases Associated with Orthopedic Injuries. Tissue Eng Part B Rev. 2020 Dec 15;26(6):571–585. Link: https://www.liebertpub.com/doi/10.1089/ten.teb.2019.0292
Kia C, Baldino J, Bell R, Ramji A, Uyeki C, Mazzocca A. Platelet-Rich Plasma: Review of Current Literature on its Use for Tendon and Ligament Pathology. Curr Rev Musculoskelet Med. 2018 Dec;11(4):566-572. doi: 10.1007/s12178-018-9515-y. PMID: 30203334; PMCID: PMC6220011. Link: https://pmc.ncbi.nlm.nih.gov/articles/PMC6220011/
Redler, Lauren H.; Thompson, Scott A.; Hsu, Stephanie H.; Ahmad, Christopher S.; Levine, William N. “Platelet-Rich Plasma Therapy: A Systematic Literature Review and Evidence for Clinical Use.” The Physician and Sportsmedicine, 2011;39(1):42-51. doi:10.3810/psm.2011.02.1861. Link: https://pubmed.ncbi.nlm.nih.gov/21378486/
