New Treatment for CRPS
Complex regional pain syndrome, more generally known as CRPS, is a condition in which pain is caused by a past event rather than improving over time; it worsens. Skin darkening and sensory alterations are just some of the other symptoms that you may begin to notice.
The severe and difficult-to-manage agony of complex regional pain syndrome must be endured. However, researchers are working hard to find novel ways to treat CRPS.
What is CRPS?
Complex regional pain syndrome is chronic pain and sensory disorder. In most instances, nerve injury causes symptoms in the arms and legs. CRPS-II is a kind of disorder.
Damage to the nerves leads the brain to send out false signals, resulting in excruciating pain that may be devastating. In most cases, the onset of CRPS occurs after an accident, surgery, stroke, or heart attack.
It was initially known as reflex sympathetic dystrophy syndrome (CRPS-I) in those patients who did not have documented nerve damage (RSD). The categorization of CRPS-I and CRPS-II patients is complicated by signs of nerve damage.
As a result, several medical professionals anticipate that CRPS will no longer be divided into two categories in the future.
Symptoms of CRPS
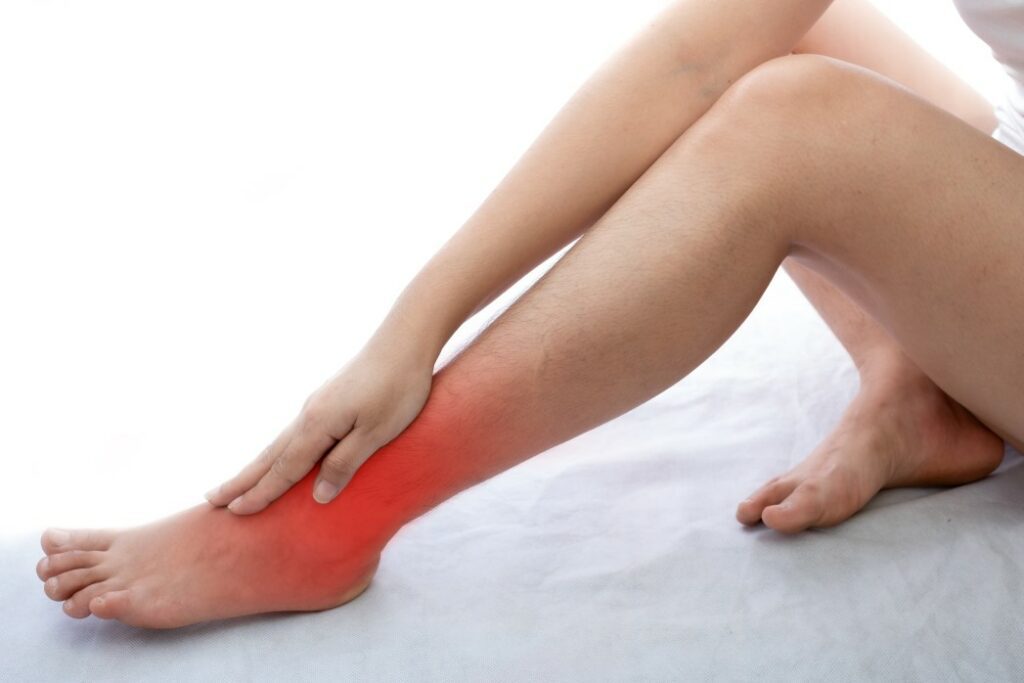
In most cases, symptoms are not present, and the number of symptoms typically decreases as the patient gets better.
- Pain that is not triggered or induced by anything else.
Some say the feeling is like being squeezed, while others describe it as "burning" or "pins and needles." Discomfort can spread throughout the whole arm or leg if the nerves are left chronically irritated for an extended period.
In some instances, it is possible to have pain and other symptoms in the opposite leg. Secondary involvement of spinal cord neurons is assumed to cause this "mirror pain" (nerve cells). Nerve damage to the mirror is less severe and eventually goes away.
- Excessive or long-lasting discomfort after usage or contact.
People with allodynia, a condition in which regular physical contact and usage are excruciatingly painful, sometimes experience increased sensitivity in the afflicted region.
Hyperalgesia is when a person experiences significant or persistent pain in response to slightly unpleasant stimuli, such as a pinprick.
- The afflicted limb swells or changes the skin's warmth, color, or texture.
Depending on the injury, the wounded limb may feel hotter or colder than the uninjured one. Blotchy, blue, purple, grey, pale, or red skin may appear on the afflicted limb.
Because of the fluctuating nature of this kind of skin symptom, it's essential to keep an eye on them. The C-nerve fibers damaged in CRPS govern the opening and shutting of the tiny blood arteries under the skin.
- Changes in the texture of the skin.
Changes in skin texture might occur over time when oxygen and nutrients aren't getting to the afflicted limb.
When it's glossy and thin in some circumstances, it's thick and scaly in other cases. As a result of this build-up, avoiding touch or cleansing, sore skin contributes.
- Nail and hair development that is out of the ordinary.
People may detect regions of intense perspiration or no sweating on the afflicted limb, and abnormal hair and nail growth may occur.
All are controlled by the nervous system and affected by the blood flow in the area.
- Inflamed or inflamed joints.
Reduced mobility causes tendons and ligaments to become less flexible, a typical condition. Internal causes of CRPS in patients who do not have exterior injuries may be caused by tight ligaments or tendons that irritate or compress nerves.
- Bone loss or growth that is too much.
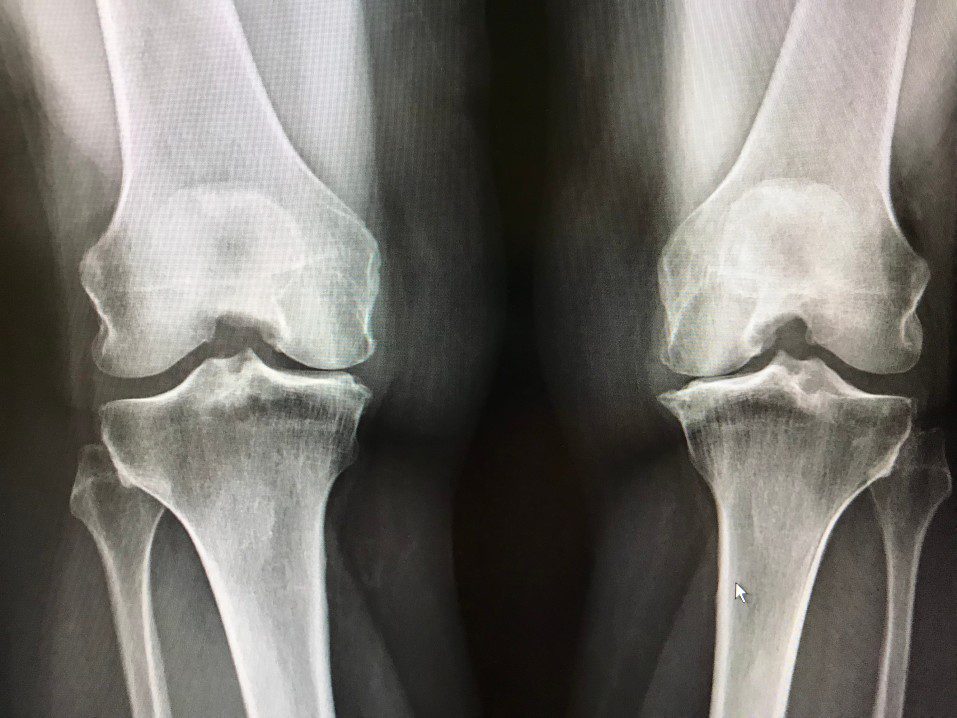
Bones that receive impulses from injured nerves are seldom impacted in CRPS-affected limbs. Experts may use X-rays or other imaging to diagnose the exact area of nerve injury and determine the most effective therapy.
Some types of bone disease, such as poorly healed fractures, or bone cysts, might irritate passing nerves and lead to or prolong the development of CRPS.
- Impaired muscular strength and mobility.
Nerve fibers that control the muscles coordinating movement are not directly damaged in most patients with CRPS. Most sufferers, however, report a decreased capacity to move the afflicted area of the body.
A few patients report dystonia, tremors, and jerks in the afflicted limbs. Usually, this is caused by pain and aberrant sensory input that aids in movement coordination. Inflammation and inadequate blood flow are also detrimental to muscle health.
These may be signs of the subsequent spread of abnormal neural activity to the brain and spinal cord. Some patients need orthopedic surgery to extend constricted tendons and restore normal flexibility and position due to their CRPS healing process.
Who can get CRPS?
This condition is characterized by nerve injury and may affect people of all ages.
However, it is more frequent among women in their 40s. CRPS is very uncommon in the elderly and youngsters under ten years old.
How is CRPS diagnosed?
No particular test can diagnose CRPS and identify a damaged nerve. The following are possible diagnoses:
- Examination by a doctor who is knowledgeable with typical patterns of sensory nerve architecture, such as an orthopedist or plastic surgeon. Patients' most aberrant skin outline frequently displays nerve damage.
- Some, but not all, of the nerve damage associated with CRPS may be diagnosed using nerve conduction testing (some injuries involve tiny nerve branches that cannot be detected this way).
- Nerve injury may be detected by ultrasound or MRI, a procedure commonly known as magnetic resonance neurography (MRN). Magnetic resonance imaging (MRI) may reveal the damaged nerve's location thanks to certain bone and bone marrow abnormalities.
- CRPS-associated increased bone resorption (the natural breakdown and resorption of bone tissue back into the body) may be seen in triple-phase bone scans (using a dye), which can aid in diagnosis and localization.
Diagnosis is more straightforward early in the condition and should not be delayed since CRPS improves with time.
What are common CRPS treatments?
Although there is no cure for CRPS, physicians and scientists are still working to find a treatment.
According to some of the most recent studies, new therapies for CRPS may be possible in the future.
Deep brain stimulation (DBS)
Electrodes are surgically implanted in the brain as part of deep brain stimulation (DBS). As a result of these electrodes, aberrant brain activity that causes pain is blocked or altered.
Physicians have used an analgesia-based strategy in the past to treat pain. According to research done at the Cleveland Clinic, it may be more effective to concentrate on the parts of the brain that normalize emotions and behavior.
In some instances, regulating the brain's emotional realm might enhance a patient's quality of life or alleviate pain-related incapacity.
Researchers have discovered a therapy option for CRPS after studying the disease's immune-system origins.
CRPS' immunological origins were investigated by a team of European experts from all over the world. Inflammation in the brain was examined, particularly in inflammatory mediators (messengers that act to promote a response).
Interleukin is a name for one of these mediators (or IL-1). IL-1 is known to activate the body's natural healing mechanisms, but there are several illnesses in which it seems to be a contributing factor.
Researchers in this study revealed that CRPS-like symptoms were induced in mice after administering antibodies from CRPS patients. Inflammation in pain-related areas of the mouse brain was a key component of transmitted CRPS.
The research team showed Anakinra, a medication that blocks IL-1, to prevent and reverse these abnormalities in mice.
According to Dr. Andreas Goebel of the University of Liverpool's Pain Research Institute, results reinforce prior findings that individuals with chronic CRPS should react well to immunological therapies.
Regenerative treatment studies show that enhanced function may be achieved.
Although regeneration treatment is still in its infancy, it has shown encouraging results in a number of trials addressing pain.
In a recent clinical trial, platelet-rich plasma is an effective treatment for carpal tunnel syndrome. Self-healing is facilitated by exposing damaged tissue to high growth factors.
A family nurse practitioner in Colorado experienced a damaged nerve on the top of her hand due to an IV started for CRPS. Due to CRPS, she could not use her hand, resulting in a lot of agony and discomfort.
Dr. Chris Centeno performed platelet lysate injections, MD of Centeno-Schultz Clinic, to break up scarring surrounding the nerve. About a month following the treatment, the patient's nerve function improves.
Throughout her therapy, she stated that she was getting better and better. Even though this is a rare incident, it may point to the need for more investigation into this therapeutic strategy.
Autoantibody reaction in complicated regional pain syndrome may be identified.
Autoantigens were identified in the skin of an afflicted limb by Veterans Affairs researchers using a mouse model of CRPS. When a patient's immune system recognizes an autoantigen as a standard protein or complex, it's called an "autoantigen."
The study's findings stated:
- Recombinant kRT16 revealed autoantigenicity, as sera from CRPS patients and fractured mice showed enhanced affinity to recombinant KRT16 protein. ""
- It's a key step in the right direction, according to researchers who believe that CRPS is an autoimmune disorder. It may open the path for additional medicines that target mechanisms rather than symptoms.
Italy has authorized the use of neridronate as a therapy for type I complicated regional pain syndrome.
The drug neridronate was recently tested in a placebo-controlled, randomized study to treat CRPS-I. A total of 82 people with CRPS-I were randomly chosen for the study.
Some were given neridronate 100 mg IV every three days (for a total of four times), whereas others were given a placebo.
After 20 days of therapy with neridronate, the visual analog scale (VAS) for pain in the neridronate-treated group was considerably lower than in the control group.
For the next twenty days, it continued to fall. Patients who received neridronate had substantial reductions in pain and heightened sensitivity compared to those who received a placebo.
What research is being done on CRPS?

The National Institute of Neurological Disorders and Stroke's (NINDS) purpose is to find a basic understanding of the brain and nervous system and apply it to minimize the burden of neurological illness.
The National Institutes of Health (NIH), the world's largest funder of biomedical research, includes NINDS, which oversees NIH's CRPS research.
In an ambitious trans-agency effort to expedite scientific solutions to reduce the national opioid public health epidemic, the NIH HEAL (Helping to End Addiction Long-term SM) Initiative has been launched.
The NIH Initiative supports pain management and therapy for opioid abuse and addiction. Over the next decade, hundreds of studies will be funded by the National Institute of Health's (NIH) Health and Human Aging Research Initiative (HEAL).
The NIH's HEAL Initiative granted grants, contracts, and cooperation agreements totaling $945 million in the Fiscal Year 2019. Visit the HEAL Initiative for more information.
NINDS-supported scientists are investigating new ways of understanding and treating CRPS and are also working to intervene to decrease the symptoms and impairment that come along with the illness.
CRPS and other painful disorders are also supported by other NIH institutions, such as the National Institutes of Health. Work on this project has included:
- There are many ways to study the acute phase of CRPS and the transition from it to the chronic phase, including genetic and other approaches to investigate the peripheral inflammatory cells, central nervous system non-neuronal cells, and the transition from the acute phase to the chronic phase, using model systems of the disease.
- To better understand the immune alterations in post-traumatic CRPS, serum and skin biopsies are examined. Further CRPS clinical trials using IVIG, rituximab B cell antibodies, and other FDA-approved therapies for autoimmune illness may benefit from these findings.
- To learn more about the processes that might help avoid chronic pain in children and adolescents with complex regional pain syndrome (CRPS), which has a better prognosis than in adults, researchers are examining the neuroplasticity of these patients.
- Transcranial magnetic stimulation (TMS) may be an effective treatment for CRPS-related pain and the accompanying cognitive, physical, and emotional problems that go along with it.
About Dr. Sean Ormond