
Coccyx pain won't go away (Is your tailbone hurting?)
The coccyx is the anatomical name for the tailbone. The sacrum is the lowest part of the spine and consists of a number of vertebral bodies that are fused together.
The tailbone, or coccyx, is the name given to the remaining little bones or ossicles below the sacrum that are likewise fused together. A fall, sitting on a hard or narrow surface, degenerative joint changes or vaginal childbirth can cause tailbone pain.
The pain in the tailbone can be dull and achy, but it usually becomes sharper when performing particular tasks, such as sitting, rising from a seated posture to a standing position, or standing for an extended period of time.
Tailbone pain can be acute, occurring for a short period of time (normally fades away on its own in a matter of weeks or months), but if it does not go away, it becomes chronic. If your coccyx pain won't go away it may be as a result of different factors, and you should visit a doctor for diagnosis and possible treatments.
Coccyx pain
Coccyx pain is also known as coccydynia or simply tailbone pain. The most common symptom of coccydynia is a dull, aching ache in the tailbone area, between the buttocks, and at the bottom of the spine.
It might be difficult to identify coccydynia due to the fact that many other conditions share the same symptoms and type of pain. Coccydynia symptoms should be checked thoroughly by a doctor to rule out any other possible causes.
Causes of coccyx pain

The tailbone has a collection of bones that make up the coccygeal vertebrae. Coccydynia can develop after an injury to the tailbone.
The coccyx is in a vulnerable position, subject to many injuries from our day-to-day activities such as simply sitting down. The most common cause of coccydynia is injury whereby the bones of the tailbone could be injured directly, such as in a fall or over time, due to repetitive activities.
The tailbone is supported by several muscles, tendons, and ligaments which could also be the trigger point for pain. The most prevalent causes of tailbone pain are sitting or standing for long periods of time.
Some of the common causes of tailbone pain include:
Poor posture: There is no definite good posture due to the unique anatomical structure of each person. There are some lifestyle habits that may, however, alter our posture in an unnatural way which may lead to coccyx pain.
Acute trauma: A sudden injury to the coccyx can cause acute pain. Most of these injuries are from falls or sports-related injuries, which be a bruise or a fracture.
Repetitive Strain Injury (RSI)/ Repeated trauma: Activities that involve repeated pressure or friction to the coccyx, such as cycling, can cause tailbone pain. This also includes sitting down for long periods of time, especially on hard no-cushioned surfaces.
Vaginal childbirth: The coccyx can be put under pressure during childbirth, especially during difficult deliveries. The ligaments may also be strained or bruised, causing coccyx pain.
Degenerative joint disease: Repetitive trauma to the tailbone can cause osteoarthritis, which is a degenerative disease, thus leading to coccyx pain.
Weight: Being overweight or underweight can lead to coccyx pain. Being overweight puts extra pressure on the coccyx, while being underweight reduces the cushioning that prevents injury to the coccyx.
Joint hypermobility: The joint between the sacrum and the coccyx and the coccyx itself is put under additional stress by hypermobility or excessive movement of the coccyx. Over-mobility of the pelvic floor can also pull on the coccyx-attached pelvic floor muscles and cause discomfort in the tailbone and the pelvis.
There are situations when the exact reason for tailbone discomfort is unknown.
Symptoms of coccyx pain
The degree of pain from tailbone injuries differs from person to person. Some people describe it as a tingling, pulsating sensation, while others experience excruciating pain that radiates to other parts of their body.
Some of the most typical signs of a tailbone injury are as follows:
Pain that worsens during activities such as sitting down, standing up, bending forward, or defecation.
- Difficulty in lying down or sleeping
- Pain during sexual intercourse
- Lower back pain or tenderness
- Increased frequency of the need to defecate
- Pain that radiates to the leg
Diagnosis of coccyx pain
As there are numerous conditions that resemble the symptoms and the sort of pain associated with coccydynia, a proper diagnosis can be difficult. Your symptoms and a physical examination of the area where the pain is would most likely lead to a diagnosis of coccydynia.
Coccydynia is a common ailment, but your doctor may also do tests to rule out other disorders with similar symptoms.
Imaging
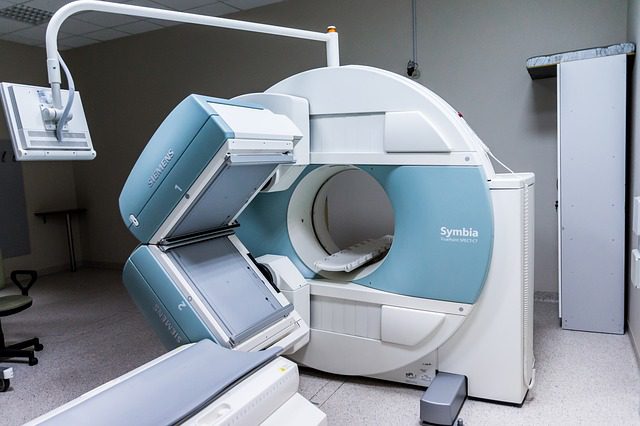
To check for fracture, imaging, such as X-rays and CT scans, is used. To check for inflammation and chordoma, an MRI or bone scan can be done.
This includes looking for other probable explanations, such as a tumor or an ingrown hair cyst that may have caused the discomfort.
Palpation
The doctor may ask you about any recent traumas, such as a fall or childbirth. An inspection of the area under pain using methods such as palpation and imaging may be used to look for any fractures, deformities, masses, or abscesses that are readily apparent (infection).
Rectal examination
Your doctor may examine your coccyx and lower spine to determine if you have a problem (sacrum). A bone spicule, a pointed new bone growth, could be the source of your pain.
The doctor holds the coccyx between their forefinger and thumb during a rectal exam where they can assess if the coccyx is too mobile by moving it. A 13-degree range of motion is considered typical.
Treatments for chronic coccyx pain

Manipulation
Through massaging the muscles attached to the tailbone, pain can be managed. It is done through the rectum.
Surgery
The coccyx can be surgically removed through a procedure known as a coccygectomy. This is typically the last line of treatment, only recommended when all other treatments fail.
Medication
You may be prescribed greater pain medication if at-home care does not alleviate your symptoms. Nonsteroidal anti-inflammatory drugs (NSAIDs) may also be prescribed by your doctor.
Injecting a steroid into the joint or ligaments in the tailbone area may also alleviate pain. Acupuncture can help alleviate pain and swelling.
A nerve block may assist in alleviating discomfort produced by the ganglion impar. It's a pain-blocking injectable that can be administered intravenously.
Antibiotics are effective in the treatment of infection, and they may also require surgical drainage.
Pain medication also helps improve other forms of treatment, such as physical therapy. When the pain is alleviated, there is more room for comfortably conducting other forms of treatment.
Physical therapy
Stretching and strengthening the surrounding muscles that support the lower back can be taught to you by a physical therapist. Proper sitting posture can be taught by your therapist as well.
Tailbone discomfort can be treated effectively and safely with physical therapy that focuses on the pelvic floor muscles. For pain relief, they may use alternating hot and cold compresses.
Reverse Kegels, a form of pelvic floor relaxation, can be used in physical therapy in order to aid in correcting the coccyx's posture. This improves the alignment of the coccyx and alleviates pain when peeing or defecating.
Coccygeal cushions
Using a coccyx pillow can help alleviate tailbone pain by reducing the pressure on the area. Cushions for the buttocks include a cutout section to ease the strain on the coccyx, which is why they're so popular.
Any sort of coccyx cushion can alleviate pain and promote blood flow in the buttock area by alleviating pressure on the tailbone in an assisted wheelchair position. Without a prescription, they can be purchased online or in stores.
Coccyx pressure is increased by circular (doughnut-shaped) cushions, which are not recommended. Rectal discomfort is a better application for them.
What to do if your coccyx pain won't go away
Coccydynia, or lower back pain that persists for more than a few days, warrants a trip to the doctor. Many additional disorders can cause the same or similar symptoms to coccydynia, some of which may be far more serious than coccydynia (such as a tailbone, hip, or spinal fracture).
To rule out other problems or begin treatment immediately, especially in cases when they are more serious, you should definitely see your doctor as soon as possible.
Your doctor should be contacted promptly if you experience any of the following symptoms: discomfort in the tailbone
- A sudden increase in swelling or pain in the coccyx region
- Frequent constipation
- Unexplained or sudden numbness, weakness, or tingling in either or both legs
- Loss of bowel or bladder control
There are some other conditions that may feel like tailbone pain but are not. They include:
- Sciatica
- Pilonidal cysts
- Infections like shingles of the buttocks
- Sacroiliitis
Prevention of coccyx pain
The easiest strategy to avoid coccydynia is to avoid injury or trauma to the tailbone, which can occur in car accidents or while participating in sports, such as football.
Your chances of suffering from tailbone discomfort can be reduced by:
Avoid falling. Maintain a clutter-free environment by picking up and tying up any stray objects or cords.
Rails should be installed on all stairways, and avoid being distracted by your phone while walking.
Avoid activities that may worsen the pain, such as cycling, horseback riding, and sitting for long periods of time.
Postpartum tailbone pain

A new mother's ability to function can be hindered if she experiences postpartum tailbone pain. When your lower back aches or pains every time you get up, it's difficult to focus on your infant.
When you sit, your tailbone aids in your balance, and it's normal to have some discomfort during labor since your body releases the hormone relaxin to soften your pelvic ligaments. Loose ligaments from your pregnancy or an injury sustained after delivery can contribute to a hurting tailbone after birth.
Your tailbone is put under additional strain by the weight of your expanding baby. It's possible that you'll feel discomfort in your tailbone because of the connection between your pelvic floor muscles and that bone.
After you give birth, your tailbone pain should go away though it's possible that you'll continue to feel the effects of a fractured or bruised tailbone for several weeks following the delivery of your child.
In order to determine the source of your discomfort, A physical examination is recommended in order to determine the source of pain. The doctor may recommend an X-ray or CT scan depending on the severity of the damage.
Frequently Asked Questions
How can I sleep with tailbone pain?
Tailbone pain is relieved when you sleep on your side though there are other measures that can improve this. Using a soft foam mattress topper or laying on your stomach with your head down on pillows that have a face carved out are options that have worked for others.
Why does childbirth cause tailbone pain?
Tailbone discomfort can occur when the spine is compressed during childbirth. The risk is increased if the delivery is complicated.
Maternal tailbone injuries may be more common in women who have a BMI above the recommended limit.
Can you exercise with an injured tailbone?
You can do this, but you should stay away from sports that could reinjure your tailbone. Sitting workouts that impose strain on the area, such as riding or rowing, should also be avoided.
Exercises prescribed by a physical therapist can aid in the recovery of an injury, and it is also suggested that you do some stretching before you begin your workout.
Can being overweight cause tailbone pain?
People who are obese are three times more likely to develop coccydynia than those who are normal weight. Tripod: Your tailbone and two buttocks help support your upper body when seated.
Coccyxes may better absorb weight when they rotate under the body, which is why it does so in thin or average-weight people. Sitting pelvic and coccyx rotation decreases with increased weight and greater buttocks.
As a result, the coccyx's tip is put under increased strain, increasing the likelihood of fracture or dislocation.
About Dr. Sean Ormond



